Hospitals, Doctors
CTRL+K
Hospitals, Doctors
CTRL+K
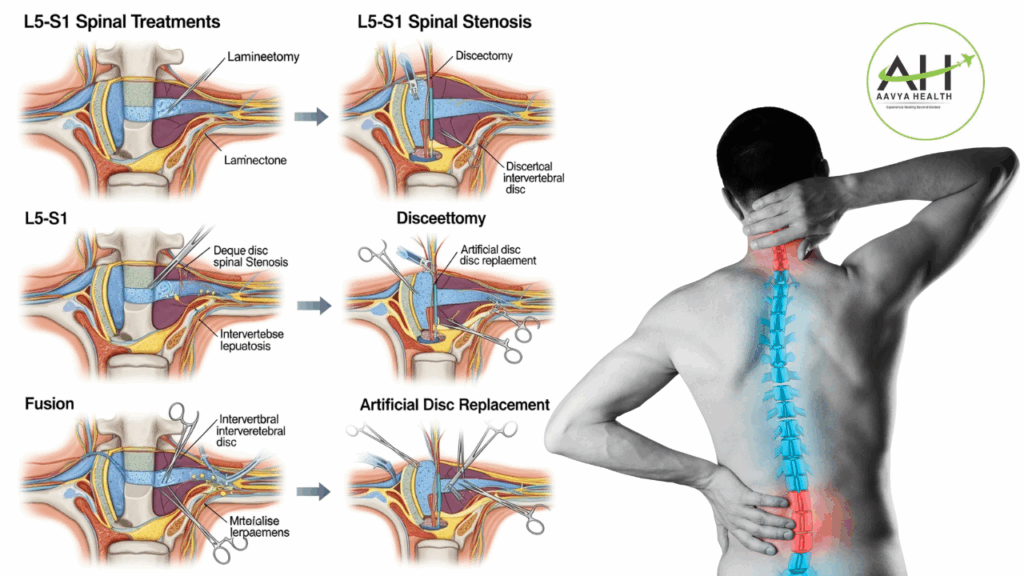
The L5-S1 segment, where the lumbar spine meets the sacrum, is a critical juncture in the human spinal column, facilitating movement and carrying much of the body’s weight. Due to its anatomical function and location, it is prone to degenerative changes and various pathologies such as herniated discs, spinal stenosis, spondylolisthesis, and chronic instability. Conservative treatments like physical therapy, medication, and injections are tried first, but surgery may be needed if these fail or neurological symptoms worsen.
Indications for Surgery at L5-S1
Surgical intervention is typically considered for L5-S1 pathology under the following circumstances:
Common Surgical Procedures for L5-S1
1. Discectomy
It involves the surgical removal of the herniated portion of the intervertebral disc that is compressing a nerve root at L5-S1. It is usually done for patients with symptomatic lumbar disc herniation causing sciatica.
Techniques:
2. Laminectomy (Decompression Surgery)
It involves removing part of the vertebral bone (lamina) and possibly adjacent ligament tissue to relieve pressure on the spinal cord or nerve roots, often due to spinal stenosis.
Indications: Especially useful in cases of central or foraminal stenosis at L5-S1, resulting in neurogenic claudication (pain, weakness, numbness with walking).
Expected Outcomes: Patients typically experience reduction in leg symptoms, with improvements in walking and standing tolerance.
3. Spinal Fusion
Spinal fusion aims to permanently join two or more vertebrae to eliminate movement at a painful segment, commonly performed for degenerative disc disease, spondylolisthesis, recurrent disc herniation, or spinal instability at L5-S1.
Techniques:
Expected Outcomes: Fusion provides stability, decreases pain from movement, and may correct deformity. Bone fusion typically takes several months. Activity restrictions are common during the healing period.
4. Artificial Disc Replacement
A motion-preserving alternative to fusion, artificial disc replacement involves removing the diseased L5-S1 disc and implanting a prosthetic device that maintains some movement.
Indications: Select cases of degenerative disc disease without significant instability, facet joint arthritis, or deformity.
Expected Outcomes: Preserves segmental motion and may allow faster recovery. Long-term data is still being collected, and not all patients are candidates.
5. Foraminotomy
Foraminotomy widens the neural foramen—the passage through which nerve roots exit the spinal canal—by trimming bone or soft tissues compressing the nerve.
Indications: Patients with foraminal stenosis causing nerve root compression at L5-S1.
Expected Outcomes: Potential for rapid relief of radicular symptoms with relatively fast recovery.
For the most successful treatment in India with a most trusted healthcare assistance partner, visit www.aavyahealth.com or WhatsApp on +91 89 2000 2010.
Pour un traitement des plus réussis en Inde avec un partenaire d’assistance médicale des plus fiables, visitez www.aavyahealth.com ou contactez-nous par WhatsApp au +91 89 2000 2010.
Surgical Approaches and Innovations
Advancements in surgical techniques have led to the widespread adoption of minimally invasive spine surgery (MISS), which uses smaller incisions, endoscopes, and specialized instruments to minimize soft tissue damage, reduce postoperative pain, and accelerate recovery.
Benefits of Minimally Invasive Approaches:
Robotic and Navigation-Guided Surgery: These technologies enhance precision in the placement of screws, cages, and implants, improving safety and outcomes.
Risks and Complications
As with any surgery, L5-S1 procedures carry potential risks, including:
Recovery and Rehabilitation
Recovery after L5-S1 surgery depends on the type of procedure performed, overall patient health, and compliance with post-operative instructions.
General Recovery Principles:
Expected Outcomes and Long-Term Prognosis
Most patients experience significant relief of leg and back pain, improved mobility, and enhanced quality of life following L5-S1 surgical interventions. Patient satisfaction rates are generally high, especially when surgery is performed for well-defined and appropriately selected indications.
Factors Influencing Outcomes:
While surgery addresses structural problems, long-term success also depends on maintaining a healthy lifestyle, ergonomic habits, and ongoing spinal care.

For the most successful treatment in India with a most trusted healthcare assistance partner, www.aavyahealth.com
Pour un traitement des plus réussis en Inde avec un partenaire d’assistance médicale des plus fiables, visitez www.aavyahealth.com ou contactez-nous par WhatsApp au +91 89 2000 2010.




Aavya Health, where our unwavering commitment to precision and excellence sets us apart as a leading medical assistance company.
As a dedicated team of professionals, we understand the significance of accurate and reliable medical assistance. Our team of skilled professionals, including medical experts, technologists, and support staff, works tirelessly to ensure that every aspect of our services meets the highest standards of quality and precision.
Whether you are seeking diagnostic support, personalized health advice, or assistance in navigating complex medical information, Aavya Health is here for you.
We strive to be your trusted partner in health, offering solutions that are not just accurate but also tailored to your unique needs.
Join us on this journey towards a healthier and more informed future, where patient’s well-being is our priority.
India is a first choice due to its world-class healthcare infrastructure, highly skilled medical professionals, advanced treatments, and cost-effective services.
You can trust us you’ll receive expert guidance and personalized support at every step in selecting the right hospital for your treatment. Because your health and well-being are our top priorities.
At Aavya Health our case manager, always prioritizes the comfort, convenience, and well-being of our international patients, and we go above and beyond to ensure that their needs are met with personalized care.
Medical treatments in India are often significantly more affordable compared to other countries, offering cost savings of up to 70% to 80% without compromising on quality or expertise.
Aavya Health case manager will streamline the process, Simply provide us with your medical needs and preferred dates, and our dedicated team will handle all aspects of appointment scheduling, travel logistics, and accommodation, ensuring a hassle-free experience for you. With our expertise and network of trusted partners, we ensure that your medical journey to India is smooth, efficient, and stress-free.
Note: AavyaHealth does not offer medical advice, diagnosis, or treatment. The services and information provided on www.aavyahealth.com are solely for informational purposes and cannot substitute professional consultation or treatment by a physician. AavyaHealth discourages copying or cloning of its webpages and content, and will take legal action to protect its intellectual property.